CALD communities need to hear the truth about COVID vaccines
Australia’s vaccine rollout appears to be on track, but a new study indicates vaccine hesitancy may be a bigger issue than previously thought.
More than one in five, or about 22 per cent, Australians say they will ‘probably’ or ‘definitely’ not get a COVID vaccine – up from 12.7 per cent in August, according to an Australian national University study.
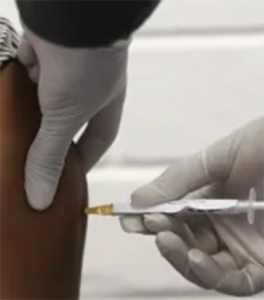 Meanwhile, more than three in 10 Australians have become less willing, with those who speak a language other than English at home, among cohorts with the most reluctance.
Meanwhile, more than three in 10 Australians have become less willing, with those who speak a language other than English at home, among cohorts with the most reluctance.
‘There is a real need to consider a significantly enhanced public health campaign in languages other than English,’ said the study’s co-author Professor Nicholas Biddle.
The Royal Australian College of General Practitioners backs up the study with anecdotal evidence.
Dr Rebecca Farley, Chair of the RACGP Specific Interests Refugee Health network, says that along with safety and efficacy concerns, cultural and religious beliefs have also worked their way into consultations, leading to questions such as ‘is the vaccine halal?’
A recent Refugee Health Network webinar also produced insights.
“The feedback from that forum was that the majority of participants wanted to get their vaccine from their GP and saw their GP as an information source of information about the vaccine,” Dr Farley said.
“Many people who aren’t yet eligible for the vaccine are already speaking to their GPs to get advice and are beginning to explore their concerns.”
But she said that what emerged during the pandemic is that many people from CALD backgrounds get much of their information from their own communities.
GPs say that diverse communities often have a distrust of authority.
They say that community leaders are an important source of information about the vaccine.
And that there is a need for engagement between state governments and CALD communities, as well as GPs, to ensure a ‘culturally responsive’ approach.
“It is really important that the insights and understanding gained from consulting and working collaboratively with different communities filters back to GPs. What are the concerns? What are the myths? What’s going on?” Dr Farley said.
She said it was important for GPs to remember that these concerns are not necessarily unique to CALD communities.
“Empathy is something that all patients need, particularly at this point in time, and … it’s partly why I do the work that I do,” Dr Farley said.
“It is so rewarding working with patients, often with interpreters and across different cultures, to really understand the things they as individuals are worried about, and as you start to really understand those things, you find that together you really can begin to address those concerns.
“It makes the difference between someone not having the vaccine, or potentially having the vaccine and still feeling very anxious and not comfortable with that decision, versus really understanding and making an informed decision to have the vaccine.
“Ensuring people have that genuine understanding of what’s going on is going to be so important as the vaccine continues to be rolled out,” Dr Farley said.
Read the ANU report here: https://csrm.cass.anu.edu.au/research/publications/change-vaccine-willingness-australia-august-2020-january-2021
Resources for addressing vaccine hesitancy in CALD communities:
- DoH COVID-19 vaccine information in various languages, including information, posters, video and social media assets
- Auslan videos on the COVID-19 vaccines
- Vaccine resources translated by the DoH for practices to display in waiting rooms, share on social media, or provide in printed form for patients
- RACGP fact sheet on telehealth consultations using an interpreter to support GPs and their patients
- The Australian Government’s Translation and Interpreting Service (TIS) has a Doctor’s Priority Line, and GPs are eligible for a free TIS code. If not already registered, general practices can register by calling 1300 131 450 or by visiting https://tisonlinetisnational.gov.au/RegisterAgency