Global health care in the balance
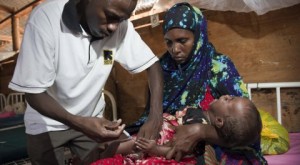
A community health worker in Kenya (Photo: International Rescue Committee)
A new push has been launched to achieve global universal health coverage with the World Health Organisation and the World Bank both listing the initiative as a priority.
Defined as “access to quality health services without the risk of financial hardship”, universal health coverage has long been a goal of community development organisations.
Global health activist Natalie Sharples has hailed the move as a step forward but warns of the challenges ahead.
“This is an exciting moment for those of us who work towards the realisation of universal health coverage, and in particular for all those who are are currently denied health care,” she said.
“But the realisation of the dream requires strong health systems, and strong health systems require health workers. But the current global shortage of 7.2 million health workers will increase to 12.9 million by 2035, with the poorest countries bearing the brunt of those shortages,” Ms Shaples said.
She said there were many causes of the global health worker crisis, including insufficient training and lack of jobs. In some countries the issue is not the overall number but their unequal distribution, typically clustered in urban areas.
Another is migration, often from low- and middle-income to high-income countries, she said.
“Five African countries – Sierra Leone, Tanzania, Mozambique, Angola and Liberia – have expatriation rates of more than 50 per cent, meaning that more than half the doctors born in those countries are now working in Organisation for Economic Cooperation and Development countries,” said Ms Sharples, a senior policy adviser at the UK-based Health Poverty Action coalition.
“This exacerbates global health inequalities, resulting in an effective subsidy from low- to high-income countries,” she said.
“In 2006 it was determined that the money saved by the UK through the recruitment of Ghanaian health workers may have exceeded that which it gave to Ghana in aid for health.”
The situation in Sierra Leone is even more dire – as the Ebola crisis has revealed. In 2010, the country had one doctor for approximately every 45,000 people, yet 27 doctors and 103 nurses trained in Sierra Leone are currently working in the UK.
“While it is not possible to quantify the losses to Sierra Leone in terms of the value of their care or in lives that could have been saved, it is possible to calculate the financial subsidy Sierra Leone is providing to the UK,” Ms Sharples said.
“Sierra Leone’s doctors and nurses – if they are relatively junior – are providing a saving of £14.5m to UK health services. If those doctors are consultants, the total subsidy from Sierra Leone to UK health services (NHS and private) could be up to £22.4m.”
A number of factors influence the decision of people to migrate, from poor pay and working conditions to the lack of opportunity for professional development.
In the case of Sierra Leone the civil war was an important factor but from the mid-1990s until the early 2000s but since then they have been attracted to the UK to fill gaps in the National Health System (NHS).
Remittances are often raised as a counter argument to compensation but money sent home provides important support for families; it does not directly compensate health systems for their losses.
The Ebola crisis has thrust the compensation debate back into the spotlight.
“There is no doubt that compensation is complex and there are numerous legitimate questions about what it would look like in practice. Who should be compensated? How could this be administered? How can we ensure it benefits the health system?” Ms Sharples said.
“Britain’s NHS depends on migrant health workers and we should celebrate their contribution. But we also need to pay the countries that trained them. It’s time that compensation was back on the table,” she said.
Sheree Peterson
AMES Staff Writer