Health system failing refugees – study says
Refugees are struggling to access Australia’s health care system because of language and cultural barriers, new research claims.
And refugees living regional Australia face even more barriers finding appropriate health care, the study said.
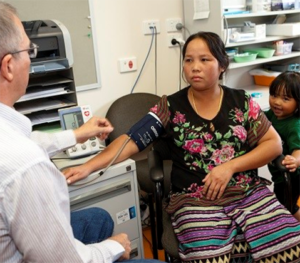 The study, by medical students at James Cook University, found that refugees struggled to understand Australia’s health care system and often ended up resorting to family, friends, word-of-mouth cures and traditional medicine.
The study, by medical students at James Cook University, found that refugees struggled to understand Australia’s health care system and often ended up resorting to family, friends, word-of-mouth cures and traditional medicine.
Sixth year medical student Michael Au led the study. He said refugees often arrived in Australia with high rates of both mental and physical health problems.
“These can be compounded by other factors including poor care in their country of origin, trauma, prolonged detention, and barriers to appropriate care on arrival,” he said.
Mr Au said the JCU team reviewed more than 1600 articles, capturing the experiences of approximately 1855 refugees in using the Australian health care system, in order to find underlying common themes in problems with refugee health care.
“The access barriers we found were largely expected – refugees had problems with the language, with how the health system worked and the differences in cultural practices they found in Australia,” he said.
As an example, Mr Au said one group of refugees expected a visit to a doctor would involve an injection, as this had been the norm in mass vaccination programs in their country of origin.
“They believed that if an injection was not given, then the GP had not satisfactorily dealt with their health issue,” he said.
Other refugees had issues with not being able to choose the gender of their doctor or the way their traditional knowledge was dismissed by clinicians.
Mr Au said the study also showed that the refugee healthcare experience was a complex interaction between how they engage with the system, how services are delivered, and the trust and privacy issues that are intertwined between them, something that had not been previously identified.
“We found that in response refugees went back to relying on their family, friends, interpreters, support workers and past experiences, and their pre-existing cultural knowledge. At times, this made it even harder to access the broader health system,” he said.
“Refugees need language support and high-quality information about how to use the healthcare system. During the re-settlement process, refugees can be overloaded with information, and oftentimes information is culturally inappropriate, not translated, or specifically targeted,” Mr Au said.
He said there was a need for further research, particularly in regional Australia.
“With no coordinated national policy on refugee health but a continued focus on resettling refugees in regional Australia, more must be learned about how to best deliver services to refugees in these settings,” Mr Au said.
He said there was a gap in the understanding of refugee health between metropolitan cities in the south and regional centres in the north.
The research revealed there was only one study examining refugee health in regional Australia, with half of the studies on the subject conducted in Melbourne alone.
“Health administrators and educators need to consider improving the cultural competency of staff and students, while policymakers need to consider engaging communities and increase professional language and cultural supports for refugees,” Mr Au said.
The study was based on a survey 1855 refugees from over 39 countries or regions.